This post originally appeared on this blog in August of 2013. It has remained one of my most viewed posts. The photos of Blake’s hands are probably the most clicked on photos in this blog, and appear at the top of Google’s Images when you search for anything related to OCD and hand washing (and they appear to be the first “real” image of what can happen to a person’s hands when contamination OCD leads to hand washing). I thought it was worth re-posting.
* Advisory: This post has some photos of hands damaged from over-washing. They may be difficult for some people to look at.
This is a nearly empty bottle of liquid soap.
It looks pretty normal sitting on the bathroom counter until you take a closer look. That brown ring around the bottom of the bottle is dirt from our backyard.
The bottle of soap caught my eye several days ago and I snapped a few photos of it to remind myself of where we’ve been. This bottle, with its dirt that is settled all around the bottom has been with us this entire summer – since before I even began this blog. It is a remnant of one of Blake’s last OCD treatment sessions before we made the heavy-hearted decision to stop therapy. I am sharing it with you today, as a way to share what Exposure and Response Prevention (ERP) can look like.
What is ERP?
ERP is “the most important therapy in CBT for OCD,” according to the International OCD Foundation. In a nutshell, ERP involves a conscious choice for a person with OCD to confront the items (thoughts, situations, etc.) that create discomfort and then not do the compulsions or rituals that would normally be provoked. The idea is for the OCD sufferer to allow his or her anxiety and discomfort to abate naturally, without using rituals to cope and thereby creating healthier ways of coping. This is commonly done with the help of a mental health therapist who is trained to do Cognitive Behavior Therapy (CBT) with OCD (for more information, Click Here. Janet at OCDtalk has also written a thorough post on ERP.).
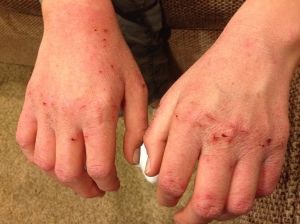
In our situation, Blake was really struggling with hand-washing compulsions (in addition to many others). It was particularly bad at the time and he ran to the sink to wash anytime he felt the slightest bit “dirty.” No amount of salves or special creams could heal the damage he was doing to his poor hands. Below are some photos of how his hands looked around the time. A reminder, these are 14-year-old hands. They are painful for me to look at. Anyone who pokes fun at compulsive hand-washing or thinks it is a joke has never lived with a family member who is suffering because of it. The pain is real, intense and it interferes with day-to-day activities.
While Blake’s treatment team had done ERP work with him on the hand-washing at the office (they would touch “dirty” things and then he would not wash), we were seeing little impact of the exposures. We all agreed at the time that Blake was “white knuckling” it through the exposure and avoiding truly immersing himself in it by reminding himself that he could wash as soon as he got home. He never gave himself the opportunity to allow his anxiety to come down to a manageable level. So, it was decided that one of his therapists would make the trip to our home. The plan was for Blake and the therapist to “contaminate” our entire house so that Blake would not have a place of safety to run to in order to avoid his discomfort.
The Day Arrives…
Blake was in agreement with the plan, until the actual day arrived. He was tired of painful hands and was hopeful that this exposure would finally put his hand-washing to rest. He greeted his therapist, happily, at the door. As they began to prepare for the actual exposure, he began to change his tune.
“I don’t remember actually agreeing to do this,” he told the therapist. His anxiety was already on the rise, and he was trying to thwart the exposure from going any further. His therapist and I reminded him of his desire to get better and advised him how important a step this was toward breaking free from the grip OCD had on his life.
Begrudgingly, he followed his therapist into the backyard where both dug into the dirt and began to put handfuls of it into a squirt bottle. Then they returned to the house where they filled the bottle with tap water and shook it vigorously. It looked like a muddy mess. I silently gulped when I saw it.
“Are you really going to spray that mess all over my house?”
This was not going to be easy – and I really have no problems with dirt. I can sit in it, get it under my nails, whatever… But this – even I wasn’t relishing the idea of my house being sprayed with a bottle of dirty water. The thing is, that was just the point. Yes, it is uncomfortable to have dirt sprayed in your house. It’s even kind of over the top. BUT, it’s not going to kill anyone. It is survivable – you can even thrive with dirt on your belongings. The point for the OCD sufferer is to stick with the discomfort long enough to recognize that it abates and that they can have a good life without having to give in to their compulsions.
Reticent as I felt, Blake’s anxiety was rising through the roof. He now wanted no part of this exposure.
“I changed my mind. I don’t want to do it,” he stated.
His therapist reminded him that this exercise, as uncomfortable as it felt right now, was going to help put his OCD in its place. She asked me to bring her all the bottles of liquid soap that were in the house. I complied and sought them out. Within a few minutes, I was back. Blake was not in a good place.
The Battle Begins
While I’d been on my mission, Blake’s therapist had opened my bottle of dish soap (which Blake uses all the time to wash his hands) and poured a good amount of that muddy water right into it. Blake was going to have none of that and before anybody could convince him otherwise, he’d dumped the entire contents of the bottle down the drain and placed the empty container in the recycle bin.
“Blake,” she reminded him, “we need to contaminate all the things you use to relieve your anxiety. You remember; we talked about this.”
“No,” he said firmly. “I don’t want to do it.”
She continued with her task and began to pour muddy water into the liquid soap bottles I had brought to her. Blake’s face grew red.
“I said, ‘No’,” he stated. “LEAVE.”
The therapist continued. She was finished contaminating his sources of washing. She took a rag and sprayed it with the dirty water.
“Come on, Blake. Help me. Let’s contaminate the house together. It’s better if you’re a part of this.”
“NO! LEAVE!” His voice was powerful. Anxiety was making way for fury.
“Remember? You wanted to get better. I’m not going to stop because I care about you. I care about your hands and I don’t want you to have to keep living with OCD bossing you around and controlling your life,” she told him.
“THERE’S NOTHING WRONG WITH ME!!!! I’M TIRED OF THIS!!! I’M TIRED OF BEING TOLD THAT I’M SICK!!! SICK! SICK! SICK! LEAVE!!! GET OUT OF MY HOUSE!!!!”
Blake was absolutely getting out of control at this point. He’d never said an angry word to his therapist before. Now, he was screaming at the top of his voice and looking like a maniac. My heart was breaking for him. I didn’t know whether to cry or burst out into giggles at the sheer anxiety the whole thing was creating in me.
His therapist continued with her quest. She carefully wiped the dirty cloth over all the furniture, the walls and our personal belongings. Our entire family was going to be in on this exposure. But was Blake going to buy into it?
Blake Hits His Breaking Point
“I TOLD YOU TO LEAVE!!! I CAN’T TAKE THIS ANYMORE!! I’M JUST GONNA…”
Blake lunged for the pencil cup on top of the cabinet near him. In one swift move, he pulled out the sharpest pair of fabric shears in the house and raised it up over his head, as if he were about to plunge it into someone. But it wasn’t clear to me if he was going for his therapist or himself.
“Put it down, Blake!” I commanded, but my words weren’t necessary. Blake’s hand hesitated in the air and his expression turned to horror and he began to tremble.
“What am I doing? What am I doing?”
He ran down the hallway to the living room where he started sobbing.
“I’m sorry. I’m sorry. I’m sorry,” he repeated.
The therapist stepped outside to call her supervisor. Blake looked at me through his tear-filled eyes.
“I wouldn’t have hurt myself,” he said. “I just wanted her to stop. I can’t believe how far I went to protect my OCD.” He cried quietly for a few minutes until his therapist stepped back into the room.
“Do you want to talk?” she asked him.
“I’m so sorry,” he said. “I wouldn’t have done anything. I know what I need to do now.”
He walked down the hallway with a half-smile on his face and picked up the abandoned squirt bottle.
“May I?” he asked.
“Of course,” she answered.
He began to make his way through the house, squirting that dirty water on the walls and the countertops. He covered his game consoles in it and his favorite sitting areas. Tears streamed down his face, but now they were tears of relief. He knew this was what he needed to be doing. Then, he directed the therapist to his room.
“We need to do my room,” he told her and he contaminated his entire room with that water, making sure he didn’t miss a thing.
The Aftermath
Blake adjusted relatively quickly to his contaminated surroundings (although I did put away all sharp objects, just in case). He didn’t care that there were pieces of dirt in the soap bottles. He relished it when I reminded him that our entire home was contaminated. He’d won another battle in the war on his OCD. His hands healed.
But the other areas his OCD affected were untouchable. He wouldn’t budge on them; held onto them like a badge of courage and battled us to keep them. Of course, this lead to us ultimately discontinuing treatment and to being in the limbo that we are in.
Today I still find remnants of that exposure, though it is about 3 months in the past. There are still places that are too high for me to reach where he aimed that squirt bottle – and I kind of like the bits of dirt that remain anyway because they remind me that we still live with contamination to some extent. They also remind me how far Blake was willing to up the ante to protect his OCD, how powerful the disorder can be in asserting itself. And I wonder when Blake will grow in his own power and desire to take it on. We can only wait and see.
Related articles
- Let’s Talk About ERP Therapy (ocdtalk.wordpress.com)